CUPS medical clinic offers a range of health services, including primary health care, opioid agonist treatment (OAT) and mental health services for Calgary’s marginalised communities. This Connecting with Care film explores CUPS’ innovative seek-and-treat model, a joint effort between pharmacist and peer worker, which is bringing hepatitis C testing and treatment to marginalised communities across the Canadian city.
Nestled between Calgary’s two turquoise rivers, the Bow and the Elbow, and in the shadow of the neighbouring Rocky Mountains Range, Canada’s fourth largest city, Calgary in Alberta, is surrounded by nature.
The city’s natural beauty is juxtapositioned against hundreds of people sleeping rough and the city’s large community of street-based drug users. Many of those who call the city home have migrated from small towns across the province and neighbouring provinces of Saskatchewan and Manitoba.
Over the past 24 years, infectious diseases specialist Dr. Gisela Macphail has become synonymous with hepatitis C care within the community and is even affectionately referred to as ‘the liver lady’ by one long-term patient, Patrick.
We started it from scratch, when a previous medical director here asked whether I would consider doing an onsite hep C clinic because only about five people per year were making it to the university (for care), yet we knew we had about 30% hep C antibody positivity. There was a huge, huge care gap.

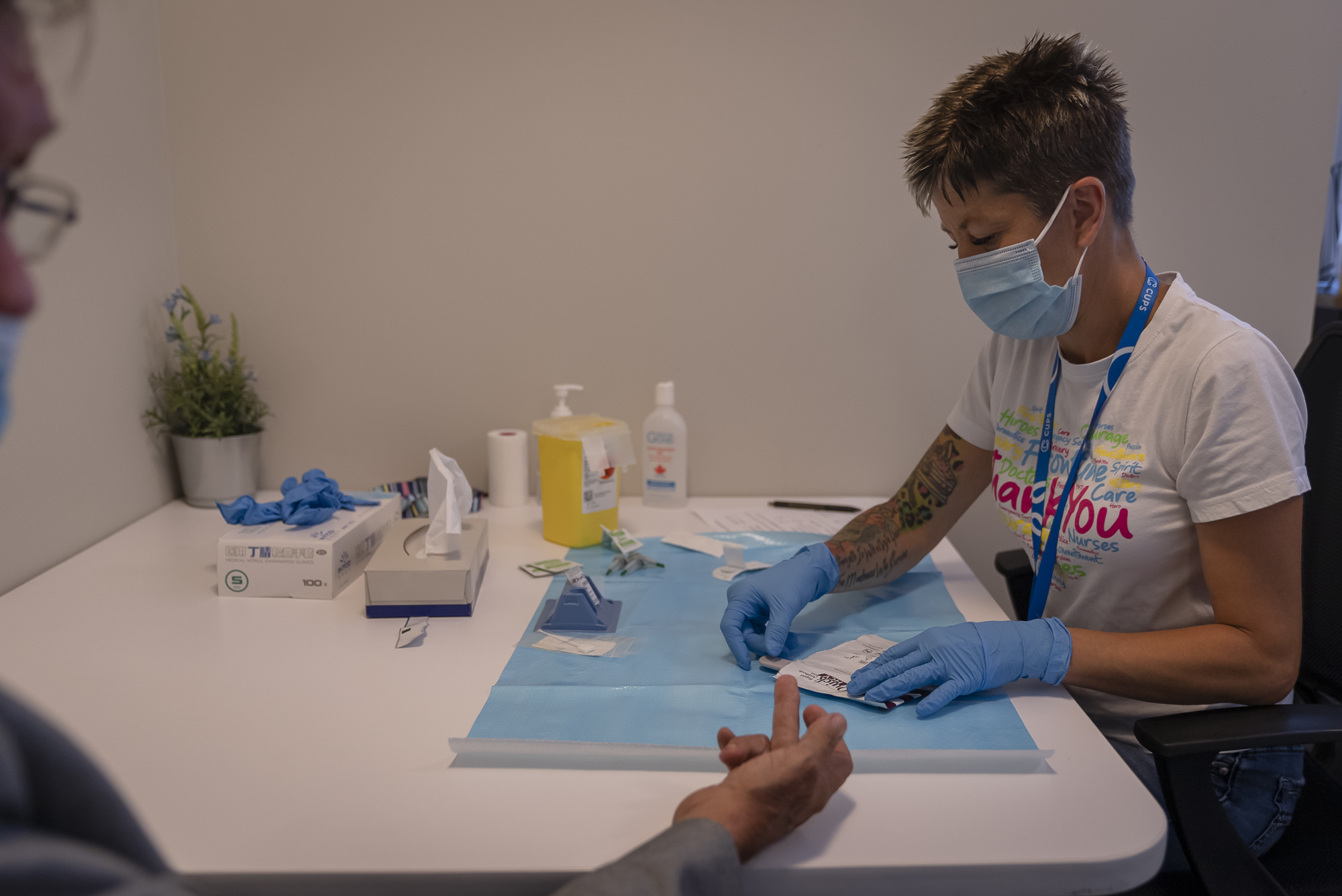
The game-changing role of CUPS medical clinic in hepatitis C treatment and care
The CUPS medical clinic offers a range of health services, including primary health care, opioid agonist treatment (OAT) and mental health services for many of Calgary’s marginalised communities. Over the past 24 years, Dr. Macphail has driven the CUPS liver clinic and overseen the hepatitis C care of hundreds of clients along with a dedicated team of nurses.
Like elsewhere, the introduction of direct-acting antivirals (DAA’s) into the Canadian province of Alberta was genuinely game-changing. Dr. Macphail, like other prescribers, was able to quickly test and treat the many people who weren’t treated with the previous interferon-based treatment.
The new medications saw an uptake in treatments and, over time, an opportunity for Dr. Macphail and her team to train other physicians and instil them with the confidence to provide care to their clients. This education was partly an acknowledgement of the significant cohort in Calgary that was not accessing hepatitis C care at the CUPS liver clinic.
The combined power of pharmacists and peer workers
The COVID-19 pandemic also provided a further reflection on the CUPS model of care and an opportunity to reflect on how CUPS could more effectively reach the hard-to-reach.
A critical shift in the CUPS model of care was when Dr. Macphail hired pharmacist and DAA prescriber Nicola Gale to work alongside her at CUPS. Nicola was already working at the Calgary Drop-In Shelter and had experience providing health care and hepatitis C treatment to some of the city’s most vulnerable community members.
DAA Treatment didn’t require as much nursing support so our focus switched from ‘how can we support other providers’, to ‘how do we even find people to engage with them’.
Nicola Gale partnered with peer worker Nicole Hibbert, and the pair were given an exciting new mandate to take hepatitis C care to the people who needed it, in the spaces they are in. This seek-and-treat model meant offering testing and treatment to people where they were, including in supported housing and shelter sites, in the drug court, at other local social services and in public spaces such as parks and along the riverfront.

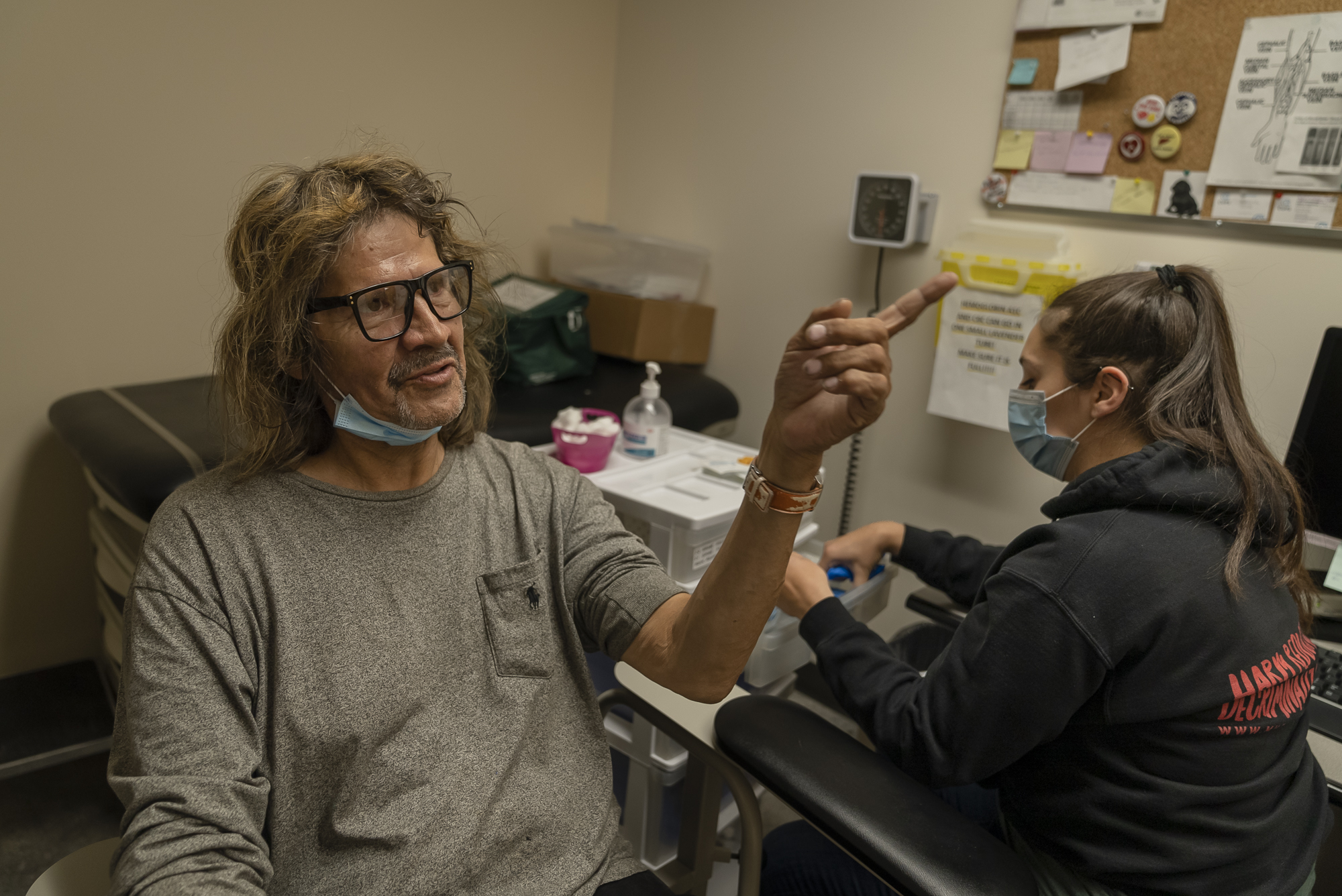
Behind the scenes of the seek-and-treat model of care
The partnership between the pharmacist and peer was incredibly successful, and the complementary skill set was clearly evident. Nicole was once a CUPS client and successfully cured her hepatitis C through the Liver Clinic. Her lived experience was evident through her natural connection with the community. Often these informal chats led by Nicole would quickly morph into a conversation about hepatitis C testing and treatment that can easily be provided by her colleague, pharmacist Nicola. And even better, it didn’t require people to come into the bricks-and-mortar clinic. Everything could be done exactly where the people were.
I love working with Nicole, she is just fantastic. I’ve learned so much from her and she has a connection with clients that I will never be able to have. Nicole has been super integral to the seek and treat model and clients love Nicole, she makes Hep C care accessible to people.
Nicole and Nicola held testing days throughout Calgary’s housing sites as part of the CUPS seek and treat model. The pair would introduce themselves to residents in the housing sites and explain they were offering a quick point-of-care hepatitis C test and the opportunity to receive treatment at home without needing to visit a doctor or pharmacist.
It was through one of these testing days that CUPS tested Patrick (quoted above) for hepatitis C. Patrick had been diagnosed with hepatitis C more than 15 years earlier during a stay in a Calgary hospital and was referred to Dr. Macphail at CUPS at the time, but decided against undergoing the available interferon-based treatment.
However, when Patrick learnt about the new DAA medication, he was prepared to undergo treatment. CUPS worked with staff at his supported housing site to ensure he could receive his hepatitis C pills and other daily medications. This approach ensured Patrick didn’t miss a day of his medication and successfully cleared hepatitis C in 2022.
The evolution of the CUPS liver clinic from a traditional hepatologist-led walk-in clinic to a pharmacist and peer-led seek-and-treat model demonstrates their commitment to the overarching goal of hepatitis C elimination within Calgary.


