Connecting with Care Sydney explores how three organisations in Sydney work together to improve the health and wellbeing of people who use drugs, focussing on the treatment and elimination of hepatitis C.
Working together to eliminate HCV
Throughout their adult life, Kim and Simon have been regulars in the inner-city suburb of Kings Cross. Over the decades, they’ve come to know the area intimately, and they’ve watched it dramatically change from the 1990s until today.
As the healthcare landscape for marginalised communities has changed over previous decades in Sydney’s inner-city, three key organisations have remained dedicated to supporting people who inject drugs.
Talking to most community members around the inner-city, they might describe the Medically Supervised Injecting Centre (MSIC) as a safe place to inject drugs, the NSW Users and AIDS Association (NUAA) as where peers provide injecting equipment and say that Kirketon Road Centre (KRC) has the best health workers.
These three services are known for providing specific services, but the reality is that KRC, MSIC and NUAA all use several approaches to provide a wide range of services centred around the health and rights of people who inject drugs.


I learnt I had Hep-C in 1988 when I got locked up in Brisbane. You do a medical as you go in, and they take your blood and then a few weeks later, I got called up to the doctor, and he says ‘well, you’ve paid the ultimate price, you’ve got hepatitis C, but you’re clear on the HIV. There is no treatment for this, and it will cause liver cirrhosis. In most people, it takes 20 years, but by 30 years, they’re dead without treatment.
Simon, Community Member.


A game-changing treatment
Since the 1990s tens of thousands of Australians like Simon have been diagnosed with hepatitis C but told there were no treatment options. In the 2000s, earlier interferon-based hepatitis C treatments were available but had low success rates and were lengthy and with significant side effects.
In 2015 the introduction of Direct Acting Antiviral (DAA) hepatitis C treatment in Australia dramatically transformed the treatment landscape for hepatitis C. This was a game-changer for services like Kirketon Road Centre, who had been providing health services to marginalised communities in the inner-city since the late 1980s but had been limited in options for people living with hepatitis C.
It meant we could be much more immediate and opportunistic about offering testing and treatment. And we could build a hepatitis C consultation into pretty much any other consultation that people came in for, because it didn’t require much preparation. It didn’t require quite so many blood tests and it didn’t require quite such a long-term commitment from both the client and the clinical staff. And so there was huge opportunity to weave hepatitis C prevention, testing, and treatment into any conversation with clients.
Dr Phillip Read, Kirketon Road Centre.
Over the past six years, as the new DAA treatments have become well established, all three organisations can offer hepatitis C testing and treatment for anyone who walks through their doors. KRC, NUAA and MSIC connect with their clients to emphasise their strengths, including being led by peers with living experience, providing an easy and free walk-in service, or offering hep C testing after using the supervised injecting facilities.
Simon and Kim have accessed services at MSIC since the early 2000’s when they opened their doors. Simon has known he’d had hep C since the late 1990s, after hearing of friends experienced with interferon-based treatments he had largely assumed hep C was something he would live with for life. Then one day, after using MSIC supervised injecting facilities everything changed for Simon.

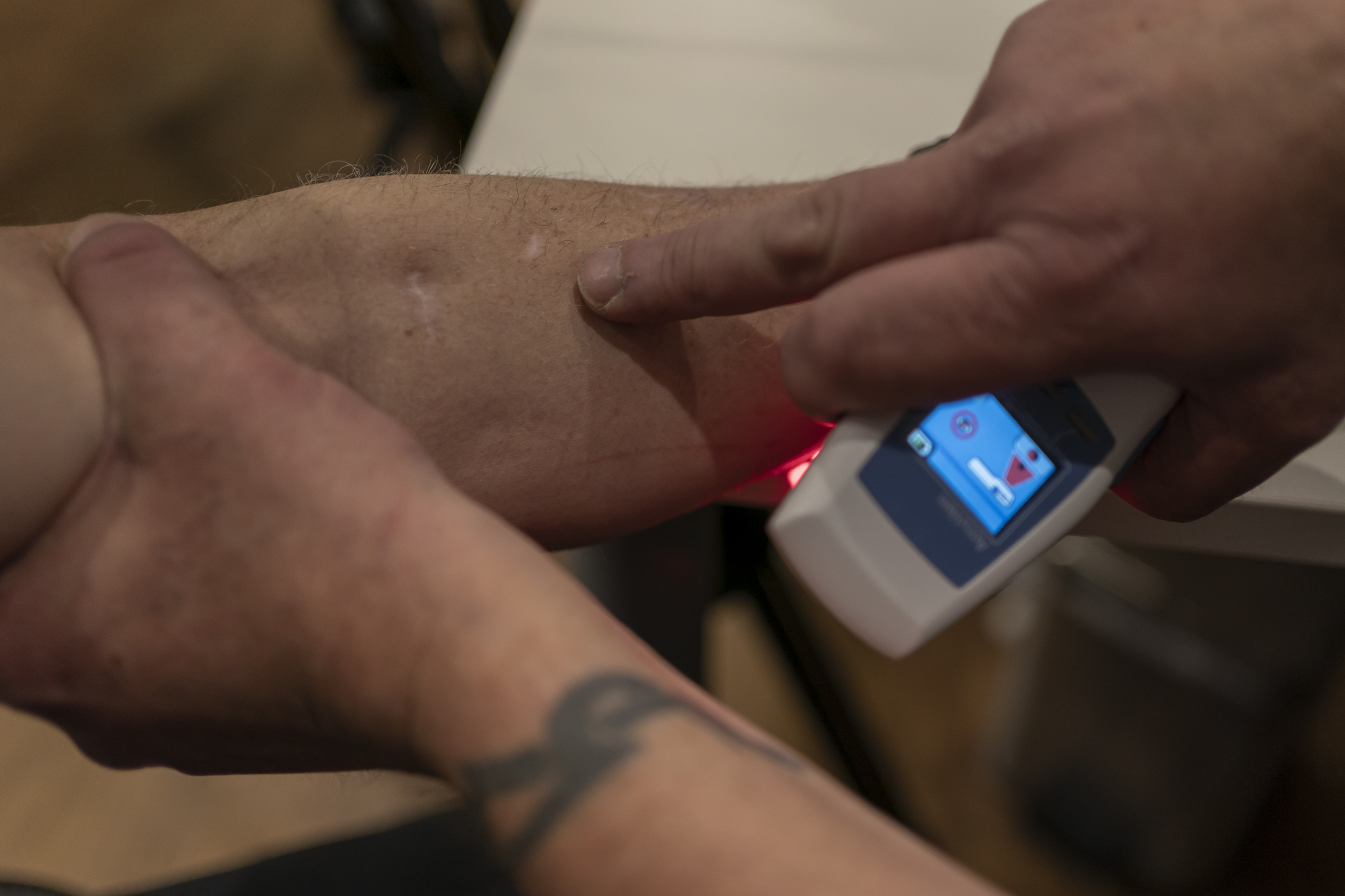
Then, in stage three, there was a sign on the wall before you exit and it said anyone interested in the Hep C program talk to Will. I asked the lady at the desk if Will was here today, and he was. He was there in a few moments, and we went straight down to the front room and did a finger prick test.
Simon, Community Member.
A few weeks later, Will asked Simon to return to MSIC, where he explained he was hepatitis C positive. Will then walked with Simon just one block up Kings Cross to Kirketon Road Centre’s building and introduced him to one of KRC’s doctors.
The doctor’s name was Dr Lucy, and she was marvellous. She explained how I shouldn’t lose any tablets, and then she gave me a packet for two weeks at a time. And each time my two weeks was up, I would go in and just say, I’m here for my tablets, and Lucy would pop up five minutes later and say here you go, Simon, it was really easy.
Simon, Community Member.

Introducing ‘Hep at Home’
After treating significant numbers of people with hepatitis C, KRC’s director Dr Phill Read believes that they’ve contributed to lowering the prevalence of hepatitis C locally.
This critical milestone has prompted the Kirketon Road Centre to adapt its model of care to engage more challenging to reach community members who haven’t yet engaged in hepatitis C care. KRC calls this new program ‘Hep at Home’ and combines their decades-long mobile outreach work with their hepatitis C treatment.
Good things come in threes
Down the road from Kirketon Road Centre and the Medically Supervised Injecting Centre in Kings Cross is the NSW Users and AIDS Association (NUAA). Everyone that walks into NUAA’s NSP to pick up injecting equipment is greeted warmly by Tony McNaughton. As a peer with living experience, Tony knows first-hand what it is like to face stigma and discrimination in health services when trying to access care.
Peers don’t have a GP. Often if they go to a doctor, it’s the emergency room, and more often than not, people don’t go to doctors because of the stigma and discrimination. I will not mince words, but it is stigma and discrimination that kills. Where I work is the opposite of that. Our mission statement is to improve the health rights, and dignity of people who use drugs. A huge number of people who access our NSP and our primary health clinic, it is probably for the first time that they’re taking their health into their own hands. Knowing that you can ask your health professional questions about your health and that you can talk about your health and that you’re not limited to a drug user because you use drugs.
Tony McNaughton, NSW Users and AIDS Association
Tony takes his job very seriously and realises the power of engagement he has as the first person a peer will talk with when they enter NUAA’s NSP. For some peers, NUAA is the only place they’ll visit to access any services because NUAA is peer-led. They know they won’t face stigma and discrimination for accessing sterile injecting equipment.
Since NUAA teamed up with KRC to establish a clinic inside their NSP, Tony is now able to directly connect peers with a nurse inside a space where they feel safe and secure. For peers who have faced repeated stigma and discrimination in health settings, accessing care inside NUAA’s NSP versus going to a different service up the road can be the difference between disengaging and connecting with care.
While KRC, MSIC and NUAA all offer different services and support to people who inject drugs, they all regularly collaborate and refer clients between services when it is in the best interest of the communities they serve.


It’s been an easy process to go from learning about the news of having Hep C to getting treatment for Hep C. It hasn’t been a tough ride at all yet and KRC has been very informative and helpful.
Jacob, Community member.
Connecting with Care Sydney shows that even within one relatively small area of a single city, there is no single model of care that works best. It results from various approaches by many organisations that provide the necessary range of support and services to people who inject drugs. All three organisations have contributed to lowering the hepatitis C prevalence in the inner-city of Sydney.
