Switzerland has some of the world’s most liberal drug policies and harm reduction services, including Heroin Assisted Treatment (HAT). There is a lot the world can learn from this small European nation, yet there are still challenges to overcome, including the need to link more people into hepatitis C testing and treatment services.
Zürich Hauptbahnhof is the largest railway Station in Switzerland and a regional hub. Just a few hundred metres away from the busy transport hub is Platzspitz, a relatively quiet park today, but it was once the site of Europe’s largest open-air drug market, with people coming from across Europe to spend time there. Unfortunately, during the 1980s and 1990s, Platzspitz became synonymous with street-based injecting drug use, large numbers of fatal overdoses and also spread in blood-born diseases, notably HIV and hepatitis C.
After significant pressure, the Swiss government responded in 1992 by closing the park. However, the Swiss response was not just the park closure but also investment into harm reduction, such as setting up needle exchanges, clean injection rooms with medical staff on hand, a methadone prescription programme, and a groundbreaking heroin prescription programme (Heroin Assisted Treatment).
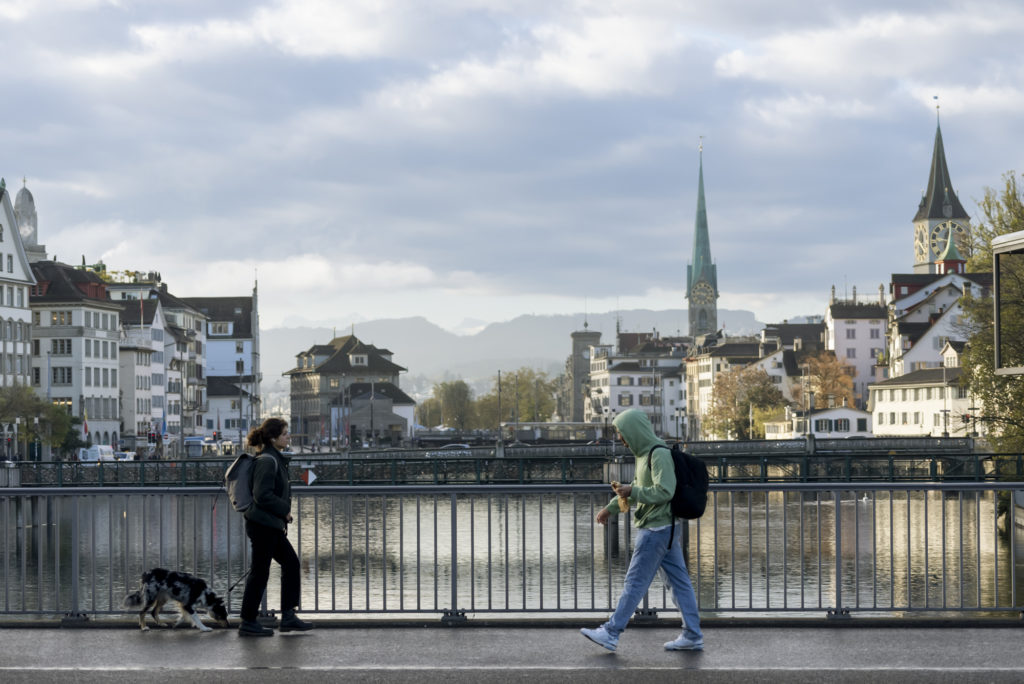
The establishment of an interdisciplinary harm reduction service
At the same time that the government closed the park, local not-for-profit Arud was established to respond to the needs of people whose substance use had become problematic.
Initially, Arud created several small clinic sites across Zürich. Over the subsequent decades, Arud has continuously expanded and further established its services and fields of action, which led the organisation to open a multidisciplinary health service under one roof in downtown Zurich in 2017.
Today, Arud is a leading institution in the field of addiction medicine. Through its work, it has played a substantial role in shaping Swiss drug policy and ensuring equitable access to the new Direct Acting Antiviral (DAA) medications to treat hepatitis C.
Dr Phillip Bruggman is an internal medicine specialist that has worked as Head of Internal Medicine at Arud since 2003. Dr Bruggman is deeply passionate about creating and maintaining a truly interdisciplinary team of professionals who can meet the many needs of their patients. Arud’s team today spans specialists in internal medicine, psychiatry, psychologists, nurses, social workers and peers.
If I have a patient who comes to me, for example, for hepatitis C treatment, but he also has mental disease disorders, I can just call Jonas, one of our psychiatrists, and he takes care of his depression. If there are social issues, I can call Yolanda, for example, one of our social workers, and she can arrange support with the patient. It’s a really interdisciplinary approach because we work very closely together.
Peer workers play an integral role
On most days of the week, Andy works on the ground floor of Arud inside the Opioid Agonist Therapy (OAT) & HAT dosing service. Andy’s experience and gentle approach as a peer worker mean he often trains and supports other peers as Arud looks to strengthen its peer workforce.
Andy is a long-time patient of Dr Phillip Bruggman, who advocated strongly to ensure Andy was one of the first people in Switzerland to access the Direct-Acting Antiviral medication to treat his hepatitis C in 2014. Being free of hepatitis C was a profound moment in Andy’s life.
Since becoming hepatitis C free, I have not used drugs or alcohol; I always say this is my second life. Phillip Bruggman is one of my mentors, he always trusts me, and he always gives me support and some comfortable feelings. And he was a great part of my journey.
community
Today, Andy is a highly treasured member of the ARUD team. He is a confident and highly competent operator of point-of-care tests and can often can be found chatting away with ARUD patients waiting to receive their OAT or HAT.
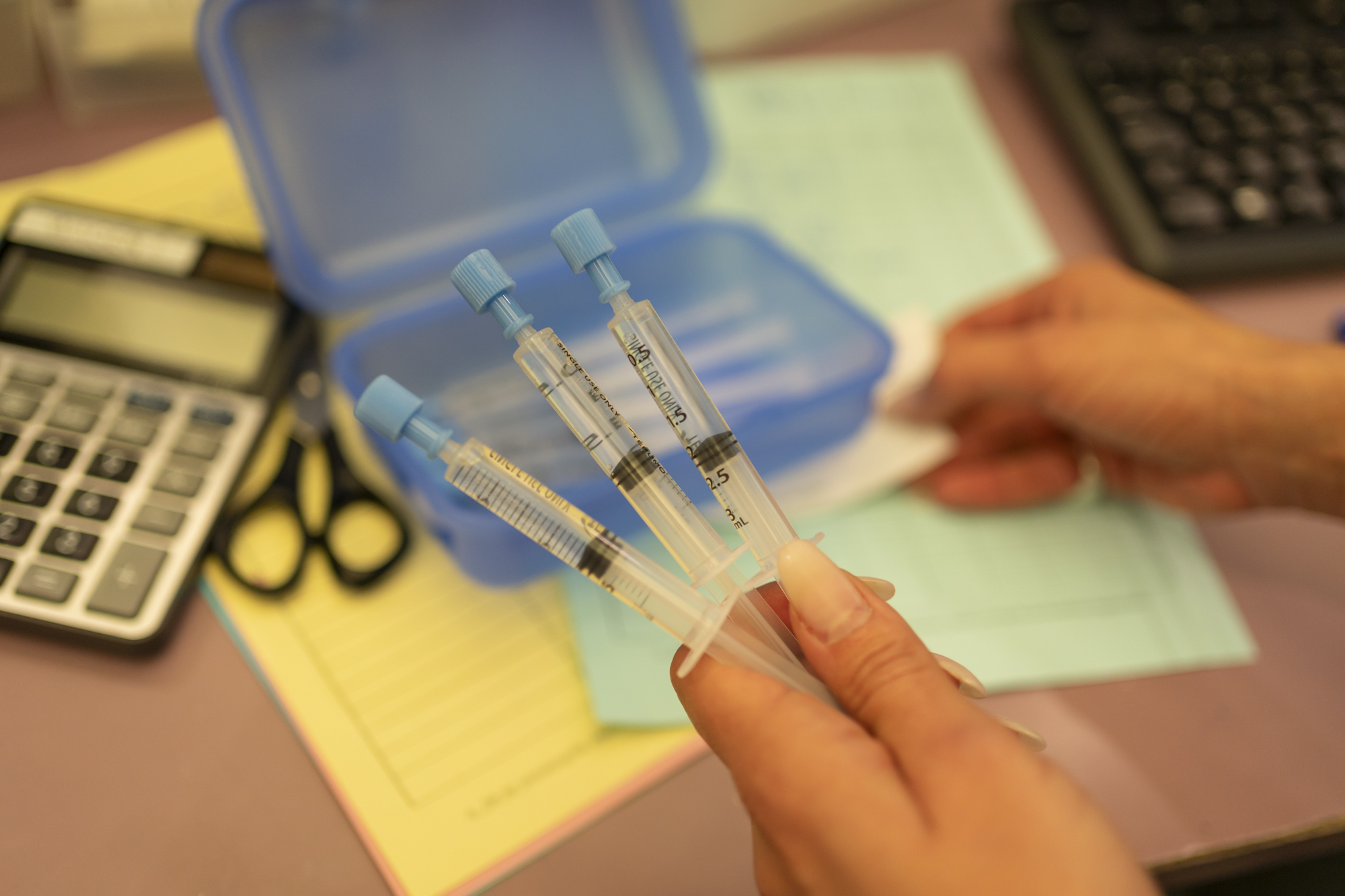
A small clinic room off the waiting room provides the perfect discreet space for Andy to invite community members with 10 minutes for a hepatitis C point-of-care test.


Various OAT treatment options are on offer, including heroin-assisted treatment (HAT)
Early each morning, Arud nurse Chonzom Yondhen and a small hard-working team of pharmacist staff and nurses open and prepare Arud’s dispensing service for the day. Arud provides a range of treatment options, including methadone, Suboxone and liquid and tablet forms of diamorphine (more commonly known as medical heroin) through the Heroin Assisted Treatment (HAT) program.
Each morning after waking up either on the streets or inside one of the city’s shelters, community member Daniel makes his way to the Arud building in downtown Zurich to visit Chonzom and receive his daily heroin dose through the HAT program.
Building trust and longevity with the community
The interdisciplinary nature of Arud means that patients like community member Robbie have maintained decades-long relationships with multiple staff members, namely Dr Bruggman and social worker Yolanda Poltera. Robbie, like many others, attempted hepatitis C treatment during the interferon era and was relieved decades later when he could finally clear the virus with the new DAA medications.
Yolanda’s office is a calming green oasis that is widely loved by ARUD’s patients. Often, when Robbie drops into ARUD each week to pick up his takeaway HAT doses, something introduced during COVID, he often heads upstairs to Yolanda’s office to discuss his ongoing broader needs.
Daniel is another community member who deeply trusts the team and utlises Arud’s nurse-managed supervised injection site. A long-time client at Arud, over the years, Daniel has built trust with the team, especially Chonzum and Dr Bruggman. This means that he has been able to engage with the team on some of his broader health needs, such as accessing hepatitis C treatment which he has now successfully cleared.
Today, ARUD continues to serve the community by offering as many services as possible in a way that is easy for people with busy lives or complex needs. ARUD has made remarkable achievements in the micro-elimination of hepatitis C among its patient group; however, Dr Bruggman understands that long-term there is still much more work needed across the small wealthy European nation.
In Switzerland we have a great healthcare system and very liberal drug policy. But still, we have a big issue when it comes to the HCV care cascade. Because OAT is prescribed by more than 50% of GP there is no integrated care, and that means that we have a lot of people still not tested. We have all the instruments ready to eliminate hepatitis C in our country, but there is still a lot of work to do.


